This is a 7-minute read.
Lymphedema is a chronic progressive disorder that results from an impaired lymphatic system. A person’s lymphatic system functions to maintain fluid balance by clearing the interstitial space of excess water, large molecules, lipids, antigens, immune cells, and particulate matter.
People with lymphedema experience a mechanical insufficiency of the lymphovascular system where fluid transport has fallen below the capacity that is needed to handle the body’s massive load of microvascular filtration. Lymphedema can be a consequence of surgical intervention, chemotherapy, radiation treatments, trauma, valvular insufficiency, and other issues.
Examining a New Patient for Lymphedema
To diagnose lymphedema, it’s essential to take a complete patient history and listen closely as the patient describes their symptoms. They may exhibit symptoms like heaviness and pressure or pain in the lower extremities, difficulty with mobility, and unilateral or bilateral swelling.
While examining the patient for clinical presentation, ask yourself: Is the swelling unilateral or bilateral? Is there symmetry or asymmetry? What does the lymphedema look like? For the physical examination, evaluate the skin and check for Stemmer’s sign and Godet’s sign, which involves inspecting the edema in the subcutaneous tissue by applying simple pressure.
Before treating the patient, do measurements that will provide a baseline for comparison post-treatment. There are a variety of different types of measurements to take, including tape, volumetric, bio-impedance, and perometry. In diagnostic testing, if needed, do imaging such as LSG, MRI/SPECT-CT LSG, DEXA, US, or NIRF.
Diagnosing a Patient With Lymphedema
The congenital form of lymphedema is Milroy’s Disease, which is also known as hereditary lymphedema and is present at birth. Primary lymphedema occurs early in life before the age of 32. Secondary lymphedema occurs when a normal lymphatic system encounters a change due to trauma, surgery, or cancer, which interrupts the lymph pathways.
When a patient has upper extremity involvement, the lymphoscintigraphy (LSG) shows the reduction of the lymph nodes on the involved auxiliary area but normal lymph nodes on the sound side. If the patient develops increased skin temperature, redness, or little blotches that look like mosquito bites, immediately make sure the patient is being treated or referred for medical evaluation for antibiotics.
Also, LSG isn’t a required diagnostic tool for lymphedema. However, if surgery is part of the patient’s treatment plan, LSG is an absolute necessity.
Conservative Lymphedema Treatments
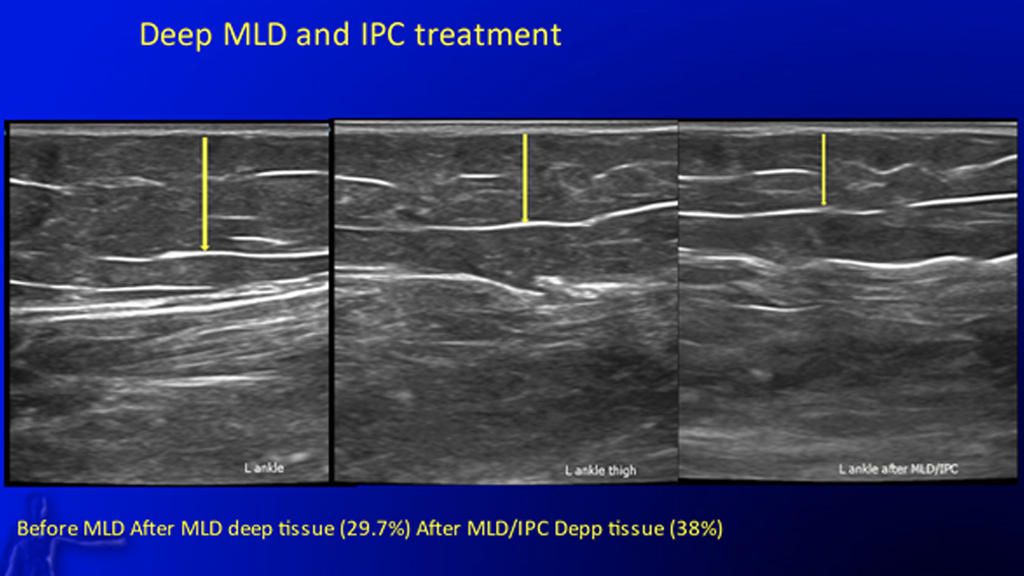
For a conservative approach to treating lymphedema, complex decongestive physiotherapy (CDP) with manual lymph drainage (MLD) and deep tissue therapy is the gold standard of treatment.
Treatment may also include the use of pneumatic compression sleeves, which are FDA-approved for use with sequential compression pumps. Compression garments should also be applied immediately after MLD treatments, and patients should follow a special nutritional guide.
Other treatments include a low-level laser, or a vibration plate, and at-home treatments like swimming, aquatic exercises, and walking.
Surgery goes beyond the most conservative treatments, but many patients experience positive outcomes. For a surgical approach to treatment, lymph-sparing liposuction has proved successful in not only reducing pain but also improving mobility.
Common Questions About Lymphedema Treatment
What is the Key to IPC Treatment?
When it comes to intermittent pneumatic compression (IPC), the hemodynamic effect is well documented. IPC increases venous flow velocity in the superficial and deep veins of the lymph using plethysmography or echo-Doppler technology.
IPC in congestive heart failure patients significantly increases the right atrial pressure and the mean pulmonary artery pressures while decreasing systemic vascular resistance in most patients without clinical worsening. One must be careful when using a pump on those with active congestive heart failure, renal failure, or pregnant women in their first trimester.
How Does Patient Compliance Impact Lymphedema?
Patients must be compliant with their treatment regimens. If they don’t adhere to their diet, exercise, compression, and self-care routines, their benefits will be fewer. Doctors and patients need to work together on treatment in a way that supports compliance.
Generally speaking, I advise that patients use the pump at home in the morning for 30 to 60 minutes, keeping the leg slightly elevated, then apply compression stockings. Over and over, I hear that the Lympha Press is easy to use, and this aids with patient compliance.
What Pressure is Recommended for the Pump?
Using the sleeve helps redistribute the pump’s flow. For a frail 80-year-old, a pressure of 40 to 45 is recommended, while a 30-year-old with stage 2 lymphedema may tolerate a pressure up to 60.
What is the Recommended Diet for Lymphedema Patients?
Dietary guidelines are not a one-size-fits-all approach. It’s common for lymphedema patients to be told to avoid sugar and dairy products, but beyond that, the doctor should work with the patient to find an individual diet plan.
Additionally, a patient must be careful if they have pre-existing conditions, as drastic dietary changes can impact those conditions. While some respond better using a keto diet, others may get better results with an anti-inflammatory diet instead.
Final Words About the Conservative Treatment of Lymphedema
Patient involvement and compliance are essential aspects of conservative, compassionate lymphedema treatment. Innovative treatment options like pneumatic compression sleeves and pumps also support the best possible outcomes for people living with lymphedema.
About Dr. Iker
Dr. Emily Iker is the director of the Lymphedema Center in Santa Monica, CA and is a physical medicine and rehabilitation specialist who focuses on the diagnosis and treatment of lymphatic disorders. She received her medical degree from St. Georgia’s University School of Medicine in Grenada and was a resident at Cabrini Medical Center and the New York Medical College. She has worked with many notable people in the field, including Dr. Robert Watanabe and Professor A. Leduc. She is a past president of the American Society of Lymphology, is board certified by the American Boards of Holistic Medicine, and founded the Lymphedema Center in Santa Monica, California.
This article has been produced in collaboration with Dr. Iker by Lympha Press, the world leader in pneumatic compression therapy. For more than 40 years, Lympha Press has provided innovative compression pump home therapy equipment that supports the best possible patient outcomes.