This is a 9-minute read.
Surviving breast cancer is a victory. Today, the 5-year survival rate for breast cancer is an astounding 90%, and the 10-year survival rate is also high at 84%. People are surviving and thriving after breast cancer.
Still, many encounter a frustrating lymphatic disorder that can occur from breast cancer treatment or from the cancer itself: breast cancer-related lymphedema (BCRL). Up to 10% of women face lymphedema after breast cancer treatment.
This article describes how lymphedema may result from breast cancer or its treatment and explores options for managing it. With proper treatment, BCRL is manageable, and new treatment options are huge strides forward for those with lymphedema.
What is Lymphedema Following Breast Cancer?
Lymphedema is the accumulation of lymph fluid due to a blockage or disruption of the lymphatic vessels, malformation of lymph vessels, or disease processes that cause the overproduction of lymph fluid. Breast cancer can disrupt the lymph vessels. Or, the treatment for breast cancer, such as surgery, removal of lymph nodes, radiation, or chemotherapy, can disrupt lymph pathways. Not everyone who has breast cancer treatment will develop lymphedema, and scientists point to factors such as an inherited defect in the lymphatic system that may predispose a patient to developing lymphedema.
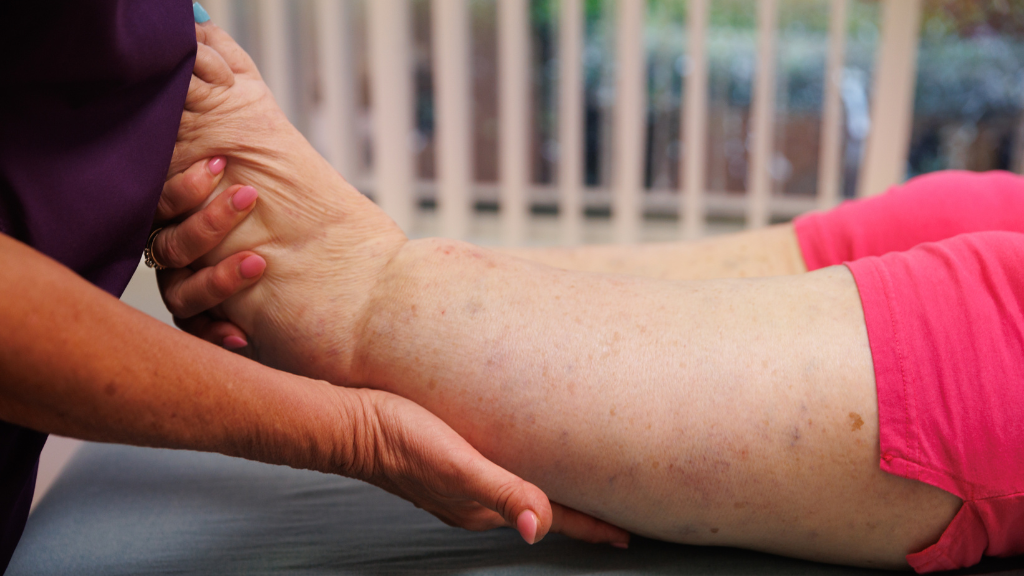
Swelling, inflammation, pain, and restricted movement of the shoulder are all symptoms that commonly arise in women with post-breast cancer lymphedema. The swelling can appear in the arm, chest, shoulder, and back.
While swelling is one of the more noticeable effects of lymphedema, fibrotic changes occur that can progress to stiffness and hardening of the tissue. Fibrosis is present in all stages of lymphedema. Patients who have had radiation treatments may experience more severe fibrosis, especially in the chest wall areas. The scarring of fibrosis is part of the body’s normal healing process but can cause permanent skin changes and can impede range of motion.
Who Develops Lymphedema After Breast Cancer Treatment?
Currently, there’s no test or method of predicting who will develop lymphedema after being treated for breast cancer. The best practice in diagnosing BCRL is evaluating the patient for the potential development of lymphedema during pre-treatment screenings, creating a holistic picture of the patient’s health, and then monitoring them during and after treatment to watch for signs of lymphedema.
Why does lymphedema occur in some people but not others? There are many answers to this pressing question, which is at the forefront of lymphedema research and innovation for scientists around the world.
In addition to breast cancer treatment, known lymphedema risk factors specific to breast cancer-related lymphedema include:
- Extensive surgery/lymph node removal
- Radiation treatments
- Chemotherapy
- Being overweight
- Family history of lymphedema or swelling, indicating a primary lymphedema or malformation of the lymphatic system or inadequate pumping response.
Lymphedema doctors and researchers are investigating a genetic and/or congenital connection, where certain people are predisposed to developing lymphedema. Although there is already a well-established type of genetic lymphedema, there may also be a genetic component to the propensity to develop BCRL.
Although there is no cure for lymphedema today, there’s cause for optimism. Breakthroughs are occurring constantly in the field of lymphedema research. Within a few decades, a cure could be on the horizon. Meanwhile, numerous lymphedema treatment options make managing the condition much easier.
Options for Lymphedema Treatment and Symptom Management
Anyone who is newly diagnosed with lymphedema should review the array of available treatment options. For lymphedema doctors and patients alike, we strongly recommend the article 7 Critical Tasks for Treating Lymphedema, which provides an in-depth look at treatment best practices, including:
- Proper wound care
- Management of expectations and understanding measures of success
- Lifestyle factors, including exercise and diet
- Innovative surgical options
- Compression garments
- Pneumatic compression
- Development of a long-term treatment plan for living with lymphedema
Combining the gold standard of CDT with other therapies is a widely accepted strategy for addressing lymphedema. Patients experience the benefits of CDT, including hands-on therapy, by an expert lymphedema therapist for the initial phase of treatment, and then can maintain the gains and further improve and reduce swelling using supportive therapies like pneumatic compression, compression garments, skin care, and mild to moderate exercise.
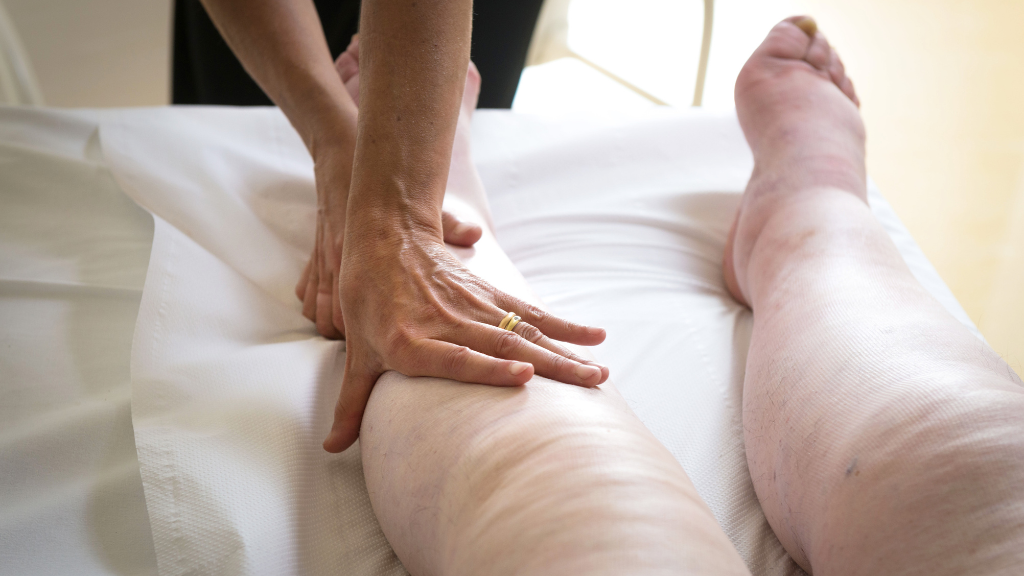
Manual lymphatic drainage (MLD) is a specialized form of massage that follows lymphatic anatomical pathways. It can be combined with exercise and pneumatic compression to increase the total benefit. Massage plus compression has shown clinically proven benefits for many patients with lymphedema.
Of course, patients should always consult a doctor before proceeding with any particular lymphedema treatment regimen, especially when it comes to treating lymphedema following breast cancer treatment. For instance, a patient’s doctor or surgeon may or may not recommend one of the latest surgical techniques for treating lymphedema depending on whether they’re a good candidate for lymphatic surgery.
Some of the latest surgical techniques include lymphatic reconstruction, lymphatic microsurgery, and lymphatic supermicrosurgery. World-renowned surgeons like Dr. Hiroo Suami and Dr. Wei F. Chen are two experts who are expanding our collective understanding of treating lymphedema through groundbreaking surgeries.
Compression Therapy for Lymphedema After Breast Cancer Treatment
Not all lymphedema treatment occurs in doctors’ offices and other clinical settings. The best ongoing care incorporates lymphedema at-home treatment where the patient is empowered to help manage their condition.
Pneumatic compression is an excellent example of an in-home solution for reducing lymphedema swelling. A pneumatic device uses a garment with air-filled chambers that inflate in a pre-programmed, sequential progression that compresses and releases the treatment area. This simulates the pumping action of lymphatic capillaries and nourishes vital fluid flow.
Research shows that women who have had breast cancer treatment experience appreciably positive outcomes by using Lympha Press compression therapy. Recently, three clinical case studies showed impressive results for patients with lumpectomies and radiation damage who used Lympha Press for lymphedema after breast cancer treatment.
Lympha Press is a type of advanced pneumatic compression device that addresses lymphedema symptoms by restoring and improving lymphatic fluid flow. It was designed to mimic the body’s natural fluid movement processes and provide a mechanical means of accomplishing a similar effect.
Clinicians and patients who are interested in learning more about BCRL treatment options can explore using Lympha Press therapy. Pneumatic compression devices offer significant lymphedema symptom relief with results that are backed by clinical studies.
For More Information About Lymphedema After Breast Cancer Treatment
After breast cancer, patients may have some hesitation to use a pneumatic compression device due to unfamiliarity with the technology and/or concerns about its comfort and effectiveness. To learn more about using this type of pneumatic compression therapy for breast cancer-related lymphedema, please see the video below, “Lympha Press: The Optimal Choice for Post-Mastectomy Lymphedema Patients”:
Lympha Press is a well-respected organization in the medical world, supplying effective lymphedema treatment devices to medical professionals and patients around the globe. In addition to supplying these devices, Lympha Press is also dedicated to providing research and support for those who are living with lymphedema.
Recently, Lympha Press welcomed Dr. Karen Herbst as its Chief Medical Officer. Dr. Herbst is one of the field’s foremost authorities on lymphatic disorders and shares the following insight into treating lymphedema: “In today’s busy world, optimizing the use of at-home intermittent pneumatic compression therapy is key for patients with lipedema, lymphedema, and vein disease.”
For more information about the latest innovative treatment options for lymphedema following breast cancer treatment, please contact Lympha Press.