This is a 9-minute read.
Pregnancy is an exciting, and maybe even slightly overwhelming, time in your life. It is marked by several new changes in your body as it grows and prepares for your new baby. For any pregnant mother, there will be many questions and considerations about your health and how it will influence and be influenced by pregnancy. This is also true for someone who is pregnant and living with lymphedema.
The most important thing to remember is that you can absolutely have a healthy pregnancy while managing lymphedema. While there may be additional challenges in the care of lymphedema while pregnant, these may be overcome through extra planning, self-care, and support from your medical providers and loved ones.
In this article, we hope to deliver information that will help you feel more informed and best prepared to manage the potential effects of pregnancy and lymphedema. More specifically, here are 3 important things to know about managing lymphedema and pregnancy.
1. Be Aware of Natural Lymphatic Changes During Pregnancy
All pregnant women, with or without lymphedema, experience a major shift in blood flow, blood volume, blood vessel workload, and hormones to support your growing child. One of these changes is a 50% increase in fluids and blood housed within your body. Your body must produce and circulate up to 20% more blood with up to a 50% increase in blood plasma volume alone.
These changes begin during the earliest weeks of pregnancy. The increased fluid volume, combined with the weight of the continuously growing placenta, uterus, and baby, adds increased pressure on the surrounding vessels, tissues, and lower extremities. This added pressure may in turn put increased stress and demand on the lymphatic system. Subsequently, this has the potential to worsen lymphedema symptoms.
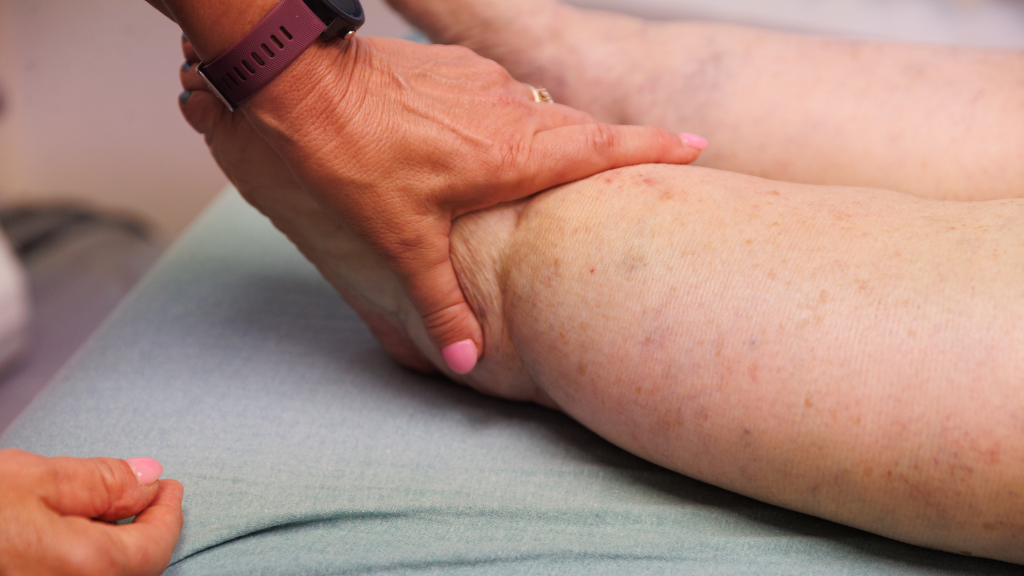
Women in the late stages of pregnancy are also at a particularly increased risk of lower-extremity edema. Because people with lymphedema are already at risk for, or are currently experiencing, lower-extremity swelling, it is important to closely monitor for new or excessive swelling in your legs as you progress through your pregnancy. If you notice new or increased lower leg swelling, contact your doctor or lymphedema therapist to determine if additional treatment is recommended. You should also feel empowered to proactively discuss concerns with your physicians to prevent and mitigate any exacerbated symptoms. Your medical team can help you plan for compression therapy, safe exercising, and healthy eating to minimize the effects of pregnancy and lymphedema.
2. Understand the Genetic Component of Lymphedema
While some cases develop due to a genetic component, having lymphedema does not mean your child will automatically develop lymphedema. Primary lymphedema is a form of lymphedema that is caused by a number of genetic variations, with symptoms emerging congenitally in childhood or into adulthood. These genetic mutations can occur spontaneously (i.e., randomly) or can be hereditary.
Although there may be a genetic component to lymphedema, the hereditary element (e.g., who will or will not inherit the genetic milieu) is not yet fully understood. Primary lymphedema is considered rare in children and only 6.5% of all lymphedema cases are congenital. The most common form of the condition, secondary lymphedema, is not caused by genetics and is strongly associated with risk and lifestyle factors such as surgery, cancer, and infections.
3. Empower Yourself By Being Proactive
Before your pregnancy, consult with your care providers to discuss what you can do to prepare. Your doctor may recommend certain exercises, a specific eating plan, or compression therapy to prepare for and maintain strong lymphatic wellness throughout your pregnancy.
During your pregnancy, you can minimize the impact of lymphedema by knowing what to expect and asking plenty of questions. In tandem with the guidance provided by your medical team, many resources highlight the use of usual lymphedema management strategies as ideal preventative measures. Some examples of these strategies include:
- Maintaining your usual routine for compression and other therapies, incorporating input from your doctors during prenatal visits
- Remaining active with gentle, low-impact exercises like yoga and water movements
- Keeping your legs elevated whenever possible to minimize the risk of lower limb swelling
Manual lymphatic drainage (MLD) therapy can also support lymphedema management during pregnancy. One study found that pregnant women who used lymphatic drainage therapy for excess lymph fluid demonstrated statistically significant changes in limb volume on therapy days versus non-therapy days. However, it is important to speak with your doctors to determine if MLD is an appropriate option for you and, if so, how to perform it correctly.
If you are traveling with lymphedema while pregnant, take extra precautions, particularly for long trips where you must sit for multiple hours. While traveling, it is important to make stops and take standing breaks for periodic movement, to rest when excess walking or standing is required, and to keep legs elevated comfortably when possible.
Pregnancy care often requires interactions with other healthcare professionals beyond your normal doctor. Ensure that any new provider you interact with during your pregnancy and birth is fully aware of your lymphedema so that they can provide appropriate, safe, and effective care. It is also important to mention new symptoms right away. Some parents choose to create a formal, written birth plan to help communicate their care and birth preferences. When developing this plan, include necessary details about your lymphedema and lymphedema management needs.
Though your care team is there to help you, lymphedema is often managed by specialists. This means that often, providers may be less informed about the condition. If you feel a care provider is unable or unwilling to address your specific pregnancy and lymphedema health needs, feel empowered to exercise your patient right to request someone new or a provider who specializes in your condition. If looking for a new lymphedema therapist near you, consult resources from organizations such as the Lymphatic Education and Research Network or the Lymphology Association of North America.
Enjoy the Excitement of Your New Baby!
Women with lymphedema can—and do—have happy, healthy pregnancies and births. You are surrounded by a large community of others who understand your situation and can provide plenty of added help and resources. Here are some posts and articles with more information to support your pregnancy journey with lymphedema:
- Family Planning and Pregnancy With Lymphedema or Lipedema (LymphCare.com)
- Lymphoedema and Pregnancy: knowing the connection, causation, and consequences (LymphConnect.co.uk)
- Pregnancy and Primary Lymphedema (Lymphnotes.com)
- Lymphoedema and Pregnancy (Lymphoedema.org)
We also invited you to explore Lympha Press resources for insights from a community of doctors and patients who understand managing lymphedema throughout pregnancy and all of life’s changes.