This is a 5-minute read.
Here’s something you might not realize about lymphedema and lymphatic disease: More people have it than muscular dystrophy, multiple sclerosis, Parkinson’s disease, ALS, and AIDS combined. Over 10 million Americans have lymphedema and lymphatic diseases, and millions more are as-yet undiagnosed. That is why knowing common lymphedema symptoms is so important.
Would you recognize the symptoms of lymphedema? If you’re not sure, please keep reading. This article shares the key warning signs of the disease plus what causes it, who tends to develop it, and options for effective treatment.
What is Lymphedema?
Before we go over the most common lymphedema symptoms, let’s go over what exactly the disease is. Lymphedema is swelling caused by an impairment of the lymphatic system. This system carries fluid and cells that help fight infections throughout the body. The impairment can happen because of congenital abnormalities, cancer or a treatment for it, or because of surgery, injuries, or other medical conditions that affect your lymphatic system or cause an overproduction of the fluid called lymph. Sometimes the onset of lymphedema develops quickly, and other times it can develop slowly over months or years.
What Are the Most Common Lymphedema Symptoms?
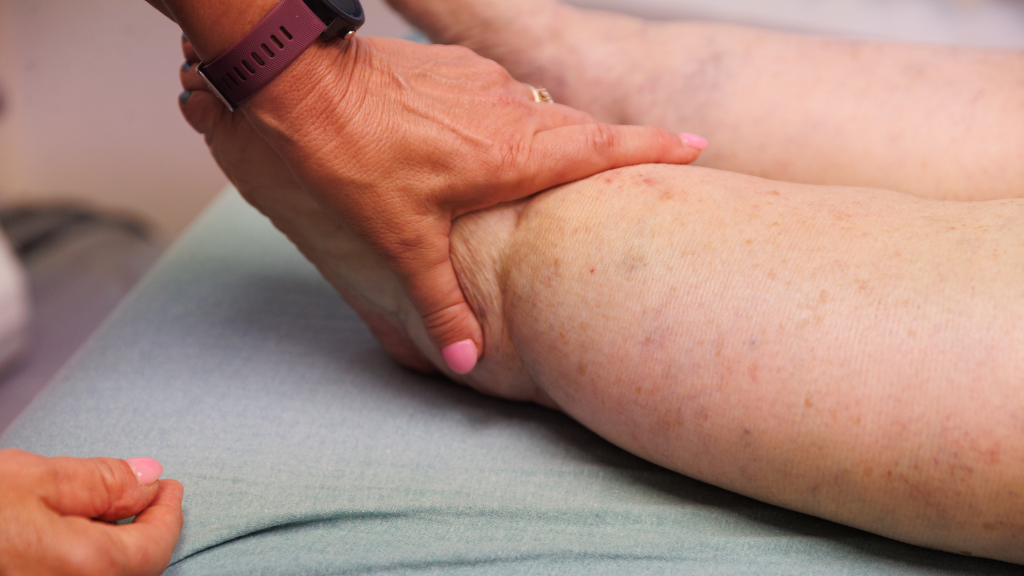
The earliest signs of lymphedema are subtle and difficult to detect. You may have a feeling of heaviness in your limbs or just a sense that something feels “off” about the sensations you’re experiencing in your limbs.
At this point, edema fluid is building up in the areas affected by poor fluid drainage.
Your lymphedema symptoms may worsen until you have noticeable swelling in your feet, legs, and arms that may or may not go away when you attempt remedies like applying compression, resting with the affected limbs raised, or laying down in bed.
Advanced lymphedema comes with more severe symptoms including extreme swelling, fluid buildup that won’t go away, skin that feels stretched and tight, open wounds, hardened tissue (known as fibrosis), restricted range of motion, and non-cancerous skin growths. People with chronic lymphedema are also at risk of life-threatening infections and sepsis.
Lymphedema progresses and worsens through four stages:
- Stage 0: Difficult to detect
- Stage 1: Reversible lymphedema
- Stage 2: Irreversible lymphedema
- Stage 3: Lymphostatic elephantiasis
Early detection of lymphedema symptoms is the key to managing the disease and preventing it from progressing to the irreversible stages. This is why it’s so important to recognize the initial warning signs of lymphedema in your own body and discuss them with your doctor.
What Causes Lymphedema and Who Develops It?
There are two main types of lymphedema: primary and secondary. Primary lymphedema involves issues with proper lymphatic system development in the body and can run in families, whereas secondary lymphedema develops due to external causes.
Injury and surgery are two of the top causes of secondary lymphedema, especially surgery and treatment related to breast cancer. Other causes include diseases such as chronic venous insufficiency, obesity, immobility, or a combination of multiple causes that may come together to trigger the development of lymphedema.
You’re more likely than the average person to develop lymphedema if you have any of the following risk factors:
- A family history of lymphedema or lymphatic disorders
- Cancer and cancer treatment, including radiation and surgery
- Any type of surgery, but particularly surgery involving the lymph nodes
- Have signs of vein disease (varicose veins, spider veins, etc.)
- Live in a country where lymphatic filariasis is endemic
- Advanced age
- Clinical obesity
Should I See a Doctor About My Lymphedema Symptoms?
If you suspect you may have lymphedema due to discovering certain risk factors or symptoms, see a doctor as soon as possible. Allowing your symptoms to persist could encourage the development of lymphedema into a more advanced stage that may be more difficult to treat.
Family doctors and other generalists aren’t always fully trained in detecting lymphedema. Seek input from a lymphedema specialist who can provide insight and advice about your condition and your best options for treatment.
Doctors may order one or all of the following tests to gain a clearer picture of the affected tissue:
- CT scan for a detailed cross-section of the body’s internal structures and evidence of potential blockages affecting the lymphatic system.
- Lymphoscintigraphy, which uses radioactive dye scanning to show movement and restrictions in the lymph vessels.
- MRI scan with magnetism and radio waves to create a high-resolution, three-dimensional scan of your tissues.
- Ultrasound for images showing obstructions inside your body’s organs and structures.
Support and Options for Lymphedema Treatment
Although there’s no cure for lymphedema, there’s plenty of reason for hope. Lymphedema is a treatable and manageable disease when you take proactive steps to support your health and seek treatment from knowledgeable medical professionals.
There are many ways you can find significant relief of your lymphedema symptoms, including a skincare routine, lifestyle and dietary changes, and using compression garments and equipment to ease your symptoms. Lympha Press compression pumps for lymphedema have been proven effective with the backing of numerous clinical studies and doctors’ recommendations.
You can also join the lymphedema community to build a network of advice and support that helps you thrive. The Lymphatic Education and Resource Network is an excellent resource and Lympha Press Lymphedema Patient Roundtables provide a wealth of trustworthy information and support.
To learn more about your lymphedema treatment options and more, you are welcome to contact Lympha Press.