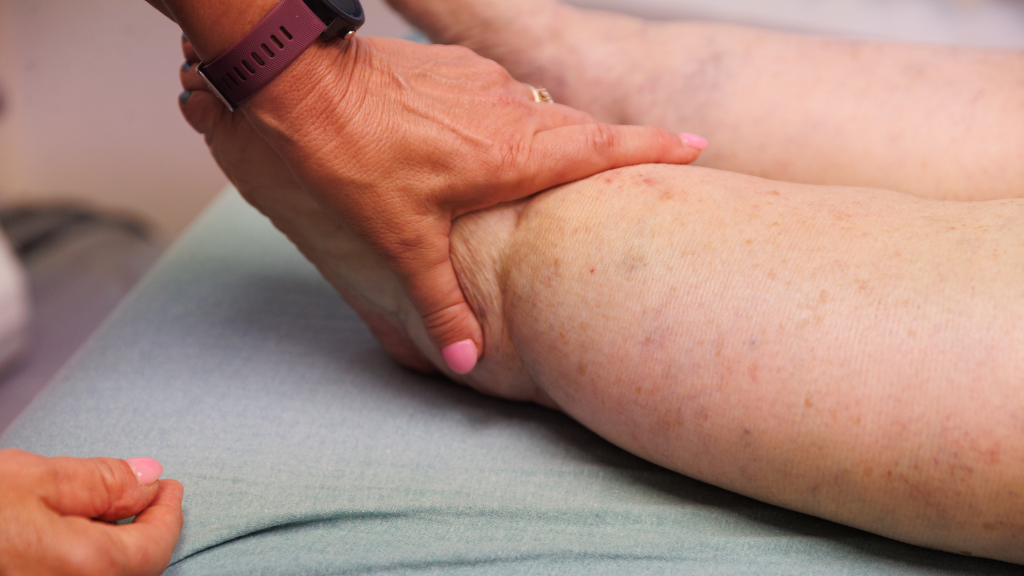
Certified lymphedema therapist Brandy McKeown, OTR/L, CLT-LANA, CLWT, explains why leg swelling may involve both chronic venous insufficiency (CVI) and lymphedema. She breaks down how these conditions overlap and why many patients go undiagnosed or undertreated. Learn key signs, risks, and treatment approaches to help you manage swelling more effectively.
Phlebolymphedema: When CVI and Lymphedema Occur Together
The combination of CVI and lymphedema is called phlebolymphedema. McKeown explains the individual conditions:
- CVI happens when the veins in the legs don’t effectively return blood to the heart. Veins become too wide, so the valves inside them don’t close completely, and blood and fluid pool in the lower legs.
- Lymphedema is a chronic buildup of lymph fluid in tissues. This condition occurs because the lymphatic system can’t keep up with the amount of fluid it needs to clear.
How CVI May Lead to Lymphedema (and Vice Versa)
“With chronic venous insufficiency, the leg veins don’t pull blood back up to the heart as well as they should, and then you can end up with extra fluid in the tissues,” says McKeown. “When the lymphatic system isn’t strong enough to keep up with the extra fluid, it can lead to lymphedema.”
Typically, CVI leads to lymphedema, rather than the other way around. However, some people already have lymphatic problems and then develop CVI in addition to lymphedema.
Why Phlebolymphedema May Be Underdiagnosed or Undertreated
McKeown says most providers receive little education about lymphedema and its overlap with CVI. A provider may recognize the venous problem (CVI) but not the lymphedema, or may diagnose lymphedema but not CVI.
“Even with an accurate diagnosis, lymphedema care is a very underserved specialty,” says McKeown. “There may not be a lymphedema therapist in rural areas. Even in metropolitan areas, the waiting list can be extremely long.”
Why Accurate Diagnosis Matters
The veins and the lymphatic system work together to clear fluid from the lower limbs. McKeown says that if phlebolymphedema is present but one component goes undiagnosed, the health consequences can be serious.
When CVI is diagnosed and treated, but lymphedema is unmanaged:
- Swelling becomes more severe, and the risk of skin ulcers (open wounds) and serious infections increases
- Venous procedures for CVI may not have optimal results because excess lymph fluid interferes with healing and increases pressure on the veins
When lymphedema is diagnosed, but CVI is missed:
- Faulty veins keep leaking fluid into tissues, making it more challenging to control swelling, even with a good management program
- Lymphedema maintenance may be frustrating due to untreated vein problems, even with lymphedema therapy
Signs of CVI and Lymphedema
There is some overlap in the signs of CVI and lymphedema. “We see patients who have significant swelling, or sometimes swelling and a wound,” says McKeown, identifying signs that can be from either condition.
CVI signs typically worsen over time and spread up the legs. They may include:
- Vein problems: Spider veins, especially little groupings on the inner ankle, and varicose veins (larger rope-like veins that swell)
- Skin changes: Darkening of the skin around the ankles (hemosiderin staining) caused by iron leaking from the blood, and thickened skin in chronically swollen areas
- Swelling in the lower legs: Swelling that may come and go at first but becomes more constant over time
Signs of lymphedema in the legs also tend to progress, especially if untreated, and may include:
- Swelling and heaviness: Swelling that worsens over time, along with feelings of heaviness or pressure in your legs
- Shape and skin changes: Changes in the shape of feet and legs, along with skin changes such as thickening
- Wounds: Open sores that are difficult to heal, typically occurring in later stages
Treatment for Phlebolymphedema
If you’re living with CVI and lymphedema, it’s critical to treat both conditions. “Just because you had a vascular procedure for a vein issue doesn’t mean you’re fixed,” says McKeown. “Your veins are doing better, but in order to ensure that those veins don’t go bad again, continued lymphedema therapy is absolutely essential.”
Phlebolymphedema treatment may include:
Vascular management
Treating the underlying venous disease is an essential first step in phlebolymphedema management. When vein function improves, less fluid leaks into surrounding tissues, reducing the burden on the lymphatic system.
Vascular management may include:
- Ablation procedures: Close damaged veins and redirect blood flow to healthier veins
- Venous stenting: Open narrowed or blocked veins to improve circulation
- Ongoing care: Monitor vein health, manage risk factors, and wear compression as recommended to prevent recurrence
Complete decongestive therapy (CDT)
CDT is the gold standard treatment for managing lymphedema. It includes:
- Manual lymph drainage (MLD): Stimulates lymph flow and moves fluid out of swollen areas
- Skin care: Protects the skin barrier through daily hygiene and moisturizing, reducing dryness, cracking, and infection risk
- Exercise: Improves circulation and helps move lymph fluid through the body
Compression therapy
Combining MLD with compression therapy can help manage swelling and increase comfort:
- Compression garments: Help control fluid buildup and support vein health after venous procedures
- Compression bandaging: Helps reduce fluid during later stages of CVI and lymphedema
- Intermittent pneumatic compression (IPC): Uses a pump and inflatable garment, such as Lympha Press, to move excess fluid and support home care
How to Talk to Your Provider About Phlebolymphedema
McKeown says that if you’ve been diagnosed with either CVI or lymphedema but you suspect you have both:
- See your primary care provider and clearly describe your symptoms
- Request a referral to a vascular specialist if you see venous signs such as spider veins, varicose veins, staining, or swelling
- Request a referral to a lymphedema therapist if you have chronic swelling or skin texture changes
Advice for Providers
McKeown stresses the importance of providers working as a team to care for patients with phlebolymphedema, as the veins and lymphatic system are so closely linked. With well-coordinated care:
- Swelling will be better controlled
- Vascular procedures will be more successful in the long term
- The risk of ulcers, infections, and disease progression decreases
“It’s really crucial that people with CVI are diagnosed with lymphedema, and lymphedema patients with CVI get the help they need,” says McKeown. “Both of these conditions benefit from a lymphedema specialist and vascular specialist working in tandem.”
Explore the Lympha Press products that can help manage phlebolymphedema at home.